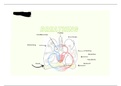
Vascular disease
Atherosclerosis
Atherosclerosis is narrowing and hardening of the arterial wall by a build-up of lipids and fibrous
materials to form a plaque. The arterial endothelium in the wall becomes damaged by high BP, DM
and smoking which allows the plaque to form. The plaque can block blood flow and lead to strokes,
organ failure or a heart attack.
This is more likely to affect the larger and high pressured vessels such as:
Coronary
Renal
Femoral
Cerebral
Carotid
Peripheral arterial disease is narrowing of the arteries in the legs caused by a plaque. Coronary artery
disease is when stable plaques form in the heart’s arteries causing angina. When this stable plaque
suddenly ruptures and clothing begins, the heart muscles begins to die causing an MI.
Cerebrovascular disease is ruptured plaques in the brains arteries causing strokes with the potential
for permanent brain damage. Temporary blockages in an artery can also cause TIAs.
There are 2 types of plaques; stable which are asymptomatic and unstable. Stable ones are when
there is plaque formation but no rupturing and no accumulation of platelets. The unstable ones are
rich in macrophages and foam cells. The extracellular matrix separating the plaque from the arterial
lumen is usually weak and prone to rupture. The rupture exposures thrombogenic material, such as
collagen to the circulation and eventually induces thrombus formation in the lumen i.e. a clot.
Atherosclerosis causes an occlusive arterial event. This is when the blood flow is reduced or blocked
in an artery. When an artery becomes occluded, these events can occur:
Ischemic stroke
TIA
MI
Acute leg ischemia
With unstable plaques that rupture, platelets begin to accumulate and aggregate. In the beginning,
when the platelets begin to gather, this only partially blocks the artery causing unstable angina.
When a thrombus comes along and binds, further blocking the artery, this causes a NSTEMI. When
the thrombus completely blocks the artery, this causes a STEMI. Once an artery becomes occluded,
tissue death (infarction) occurs within 5 minutes. Death can occur within an hour of symptom onset.
Triggers for plaque rupture:
Physical exertion
Pulse rate
Blood pressure
Vasoconstriction
Risk factors:
Modifiable
, o Diabetes or impaired glucose tolerance
o Hyperlipidaemia
o Hypertension
o Smoking
Non-modifiable
o Advanced age
o Male gender
o Family history
o Genetic abnormalities
Others
o Hypercoagulability
o Post menopause
o Hyperthyroidism
o Sleep disorders
Symptoms:
Chest pain
SOB – worst on exertion
Peripheral vascular disease
o Pallor/cyanosis
o Skin ulcers
o Muscle weakness
o Confusion
Investigations:
FBC, U&E, HbA1c and lipid profile
Ankle-brachial index
o Tells us if you have it in your legs and feet
o Abnormal difference may indicate peripheral vascular disease
ECG
US if peripheral vascular disease is suspected
Treatment:
Acute
o Percutaneous coronary intervention (PCI) e.g. stent
o CABG
o Thrombolysis e.g. alteplase
Medications
o Calcium channel blockers e.g. amlodipine
o Ace inhibitors e.g. lisinopril
o Beta blockers e.g. bisoprolol
o Antiplatelets e.g. aspirin
Prevention
o Statins e.g. atorvastatin
Peripheral arterial disease (PAD)
Atherosclerosis
Atherosclerosis is narrowing and hardening of the arterial wall by a build-up of lipids and fibrous
materials to form a plaque. The arterial endothelium in the wall becomes damaged by high BP, DM
and smoking which allows the plaque to form. The plaque can block blood flow and lead to strokes,
organ failure or a heart attack.
This is more likely to affect the larger and high pressured vessels such as:
Coronary
Renal
Femoral
Cerebral
Carotid
Peripheral arterial disease is narrowing of the arteries in the legs caused by a plaque. Coronary artery
disease is when stable plaques form in the heart’s arteries causing angina. When this stable plaque
suddenly ruptures and clothing begins, the heart muscles begins to die causing an MI.
Cerebrovascular disease is ruptured plaques in the brains arteries causing strokes with the potential
for permanent brain damage. Temporary blockages in an artery can also cause TIAs.
There are 2 types of plaques; stable which are asymptomatic and unstable. Stable ones are when
there is plaque formation but no rupturing and no accumulation of platelets. The unstable ones are
rich in macrophages and foam cells. The extracellular matrix separating the plaque from the arterial
lumen is usually weak and prone to rupture. The rupture exposures thrombogenic material, such as
collagen to the circulation and eventually induces thrombus formation in the lumen i.e. a clot.
Atherosclerosis causes an occlusive arterial event. This is when the blood flow is reduced or blocked
in an artery. When an artery becomes occluded, these events can occur:
Ischemic stroke
TIA
MI
Acute leg ischemia
With unstable plaques that rupture, platelets begin to accumulate and aggregate. In the beginning,
when the platelets begin to gather, this only partially blocks the artery causing unstable angina.
When a thrombus comes along and binds, further blocking the artery, this causes a NSTEMI. When
the thrombus completely blocks the artery, this causes a STEMI. Once an artery becomes occluded,
tissue death (infarction) occurs within 5 minutes. Death can occur within an hour of symptom onset.
Triggers for plaque rupture:
Physical exertion
Pulse rate
Blood pressure
Vasoconstriction
Risk factors:
Modifiable
, o Diabetes or impaired glucose tolerance
o Hyperlipidaemia
o Hypertension
o Smoking
Non-modifiable
o Advanced age
o Male gender
o Family history
o Genetic abnormalities
Others
o Hypercoagulability
o Post menopause
o Hyperthyroidism
o Sleep disorders
Symptoms:
Chest pain
SOB – worst on exertion
Peripheral vascular disease
o Pallor/cyanosis
o Skin ulcers
o Muscle weakness
o Confusion
Investigations:
FBC, U&E, HbA1c and lipid profile
Ankle-brachial index
o Tells us if you have it in your legs and feet
o Abnormal difference may indicate peripheral vascular disease
ECG
US if peripheral vascular disease is suspected
Treatment:
Acute
o Percutaneous coronary intervention (PCI) e.g. stent
o CABG
o Thrombolysis e.g. alteplase
Medications
o Calcium channel blockers e.g. amlodipine
o Ace inhibitors e.g. lisinopril
o Beta blockers e.g. bisoprolol
o Antiplatelets e.g. aspirin
Prevention
o Statins e.g. atorvastatin
Peripheral arterial disease (PAD)