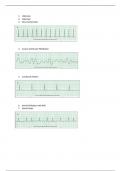
OB FHR Assessment PPT
110-160 bpm - normal FHR = -fetal bradycardia -fetal tachycardia -absence of FHR variability -late decelerations -variable decerelations - associated with fetal hypoxia 160 infection, distress, maternal factors -infection of chorioamnitis -maternal dehydration -fetal anemia (rh incompatability) -street drugs (cocaine) - fetal tachycardia 110 bpm congenital abnormalities, distress - fetal bradycardia -acid base imbalance (acidodic) -no fetal reserve -hypoxic **check maternal medication (opioids, sedatives), fetal hypoxia and acidemia, when babies in sleep cycle **should NOT last more than 30 mins - absence of variability contractions - compress + suppress blood flow detect baseline rhythm and increase or decrease in FHR *gives basic rate, no variability - auscultation FHR ultrasound - measures FHR measures uterine activity - toco transducer -if mom ruptures -ambulation: check before walking and check after -pain med or changing dose: check before and after med is given -reassess when pain med is at its peak levels -after vag exams -insertion of catheters - when to check FHR -accurate, internal FHR monitoring -helpful for obese patients and those that are difficult to externally monitor (polydramnios, IUGR, multiples) - fetal scalp electrode measures the strength of contractions in mm Hg -internal monitor -sits in amniotic fluid -depicts frequency, duration, and strength of contractions *either mom or baby is at high risk - intrauterine pressure catheter (IUPC) all it tells us is the rhythm and increase and decrease, gives basic rate, no variability -latent: every 30-60 mins -active: every 15-30 min -second stage: 5-15 min *methods: doppler + fetoscope, meant to pick up FHR only - intermittent auscultation gives you the variability -ultrasound: FHR -toco: transducer, uterine activity -IUPC: contraction strength *WHO: receiving oxytocin, concern with placenta previa, post date, meconium stained fluid, abnormal non stress test -internal, in amniotic fluid - continuous auscultation -whenever mother membranes rupture -change in meds, before, after, and peak med level -when mother ambulating: before and after -vag exam -foley - intermittent FHR monitoring any mother who received oxytocin -risk for previa -IUGR -abnormal NST -fetal distress - continuous FHR monitoring 110-160 bpm *ideal = 130-140 bpm - normal baseline FHR = evaluated over 10 minutes and between contractions -documented as a range - baseline FHR -absent -minimal (5 beats) -moderate (6-25) NORMAL -marked (25+) - variability -decrease in FHR occurring with contractions -onset occurs before contraction peak -recovery to baseline rate occurs by contraction end *possible cause: fetal head compression - early decelerations -decrease in FHR occurring with contraction -onset with of after peak of contraction -recovery to baseline occurs after contraction ends *affects blood flow to the placenta - late decelerations decreased uteroplacental blood flow/oxygen -vena cava syndrome, hyper stimulation of uterus -preeclampsia, hypertension, diabetes, anemia, chronic maternal disease *vascular disease and placental problems - late decelerations etiology -turn mom on side lying -start IV -turn off oxytocin (Pitocin)/hyperstimulation -O2 mask 8-10 L for baby -notify hep - nursing interventions for late decelerations decrease in FHR occurring without regard to contractions -range from mild to severe -shaped like "V" or "W" -less than 15 seconds and 15 beats below baseline - variable deceleration cord prolapse, cord compression - variable deceleration probable causes /etiology -mom to side lying position , knee chest position -O2 by mask -vag exam -amnioinfusion (infuse NS for more fluid, pressure of the cord) by Cath in uterus - variable decelerations nursing interventions (cord prolapse)
Written for
- Institution
- Rnc OB
- Course
- Rnc OB
Document information
- Uploaded on
- October 16, 2024
- Number of pages
- 7
- Written in
- 2024/2025
- Type
- Exam (elaborations)
- Contains
- Questions & answers
Subjects
Also available in package deal